Relevance: UPSC GS Paper III: Science and Technology, biotechnology, industrial growth, supply-chain resilience, pharmaceutical sector
For Prelims:
- Active Pharmaceutical Ingredients (APIs), Key Starting Materials (KSMs), Production Linked Incentive Scheme, Biopharma Shakti, CDSCO, SUGAM Portal, Indian Pharmacopoeia 2026, Biosimilars, Zero Liquid Discharge, Jan Aushadhi Kendras, Medical Device Classification, NPPA
For Mains:
- Innovation-led pharmaceutical growth, regulatory harmonisation, API dependency, R&D gap, biosimilar leadership, supply-chain resilience, pharma exports, quality assurance, ESG compliance, pharmaceutical sovereignty, value-based pricing, AI-led drug discovery
Why in News?
India’s pharmaceutical sector is entering a decisive phase of transformation. The sector, which is valued at nearly $65 billion, supplies around 20% of the world’s generic medicines. India now aims to build a $130 billion pharmaceutical market by 2030.
The recent debate highlights that India’s next pharma leap will not depend only on low-cost manufacturing. It will depend on science-led innovation, strong regulatory systems, global harmonisation of standards, and higher investment in biopharmaceutical research.
Background and Context
For many decades, India has been known as the “Pharmacy of the World” because of its ability to manufacture affordable generic medicines. This model helped India provide low-cost medicines to domestic and global markets.
However, the global pharmaceutical industry is now moving towards complex products such as biosimilars, biologics, mRNA vaccines, cell therapies, gene therapies and precision medicine. These products require strong research capacity, skilled human resources, high-quality manufacturing and globally trusted regulatory systems.
Therefore, India is now trying to move from a volume-based generic model to a value-based innovation model. In this transition, regulation is no longer only a compliance issue. It has become an important part of economic infrastructure.

India’s Emergence as a Global Pharmaceutical Powerhouse
- Shift from Generic Manufacturing to Biopharmaceutical Innovation
- India is gradually moving from simple generic drug manufacturing towards advanced biopharmaceutical innovation. This shift focuses on frontier biologics, novel molecules and high-value therapies.
- The launch of Biopharma Shakti in the 2026 Union Budget is an important step in this direction. It is a ₹10,000 crore initiative aimed at supporting new national institutes and creating 1,000 accredited clinical trial sites.
- This can help India build a stronger research ecosystem and reduce dependence on foreign innovation.
- Growth in Biosimilars and Complex Therapies
- India is becoming an important player in biosimilars and complex therapies. Biosimilars are biological medicines that are highly similar to already approved biological drugs. They are useful in treating chronic diseases such as cancer, autoimmune disorders and diabetes.
- India has more than 100 approved biosimilars and is also progressing in advanced areas such as Antibody-Drug Conjugates (ADCs) and CRISPR-based innovations.
- The domestic biosimilars market is projected to grow significantly, showing India’s ability to combine affordability with advanced science.
- Supply Chain Autonomy through PLI Schemes
- India has historically depended heavily on imports for Active Pharmaceutical Ingredients (APIs) and Key Starting Materials (KSMs). This dependence became a major concern during global supply-chain disruptions.
- The Production Linked Incentive Scheme for pharmaceuticals aims to reduce this dependence by encouraging domestic production of critical APIs.
- By late 2025, the scheme helped establish an annual production capacity of 55,100 metric tonnes for 26 critical APIs. This is important for India’s pharmaceutical sovereignty and health security.
- Regulatory Modernisation and Faster Approvals
The Central Drugs Standard Control Organisation (CDSCO) is modernising its regulatory framework. India is moving towards digital-first, risk-based and science-driven approvals.
Recent reforms include:
- Dossier-based licensing system
- Faster No-Objection Certificates for laboratory testing
- Automated services through the SUGAM portal
- Inclusion of new vaccines and blood products in the Indian Pharmacopoeia 2026
Such reforms can reduce delays, improve transparency and make Indian regulation closer to global standards.
- AI-Driven Drug Discovery
- Artificial Intelligence is becoming important in drug discovery. It helps in faster identification of drug targets, molecular design, clinical data analysis and prediction of drug behaviour.
- India has a strong advantage because of its digital talent and growing biotechnology base. AI-native platforms can help Indian firms reduce the time and cost of drug discovery.
- This can support the transition from one-time product research to reusable technology platforms.
- Strong Export Performance
- India’s pharmaceutical exports continue to grow. India exports medicines to 191 countries, and a large share goes to regulated markets such as the United States and Europe.
- This shows that India is already an important part of the global healthcare supply chain. However, continued access to high-value markets will depend on strict quality standards and regulatory credibility.
- Medical Device Manufacturing and Classification
- India is also trying to strengthen its medical device sector. The regulatory framework is being aligned with risk-based global standards.
- In 2025–26, the CDSCO reclassified 553 medical devices based on risk. High-risk devices were placed in the stricter Class D category. The Bureau of Indian Standards also moved towards faster certification norms for important healthcare devices.
- This can help Indian manufacturers become more export-ready.
- Universal Access through Jan Aushadhi Kendras
- India is also expanding access to affordable medicines through Jan Aushadhi Kendras. By March 2026, more than 18,646 Jan Aushadhi Kendras were operational.
- These centres provide affordable medicines and medical devices, helping reduce out-of-pocket expenditure for citizens.
- Thus, India’s pharma strategy has two sides:
first, global pharmaceutical leadership; second, affordable medicine for citizens.
Major Challenges Confronting India’s Pharmaceutical Sector
- Dependence on Imported APIs and KSMs
- India still imports a large share of its API requirements. This is especially serious in areas such as antibiotics and fermentation-based KSMs.
- Although PLI schemes have improved domestic production, India continues to face challenges in scaling advanced fermentation technology. This creates vulnerability in the supply of life-saving medicines.
- Quality Assurance and Global Credibility Issues
- India’s pharmaceutical brand faces challenges due to quality-related concerns. Import alerts, warning letters and contamination incidents affect India’s image in global markets.
- For a country that wants to lead regulated markets, quality assurance must become non-negotiable. Strong inspection systems, data integrity and manufacturing discipline are essential.
- Low Investment in R&D
- Indian pharmaceutical companies still spend less on research compared to global innovators. Most firms continue to focus on generics rather than high-risk areas like New Chemical Entities (NCEs) and advanced therapies.
- This limits India’s ability to become a true innovation leader. Without strong R&D, India may remain dependent on foreign discoveries.
- Price Controls and Rising Input Costs
- The National Pharmaceutical Pricing Authority (NPPA) controls the prices of essential medicines. This helps protect consumers, but it may also create pressure on manufacturers when raw material costs rise sharply.
- If prices are too rigid, some MSMEs may find essential formulations economically unviable. Therefore, India needs a balanced pricing framework that protects both affordability and industrial sustainability.
- Cybersecurity and Data Integrity Risks
- As pharmaceutical firms adopt AI, digital platforms and automated manufacturing, cybersecurity risks are increasing. Cyberattacks can affect intellectual property, clinical trial data and manufacturing continuity.
- For a science-led pharma sector, data security is as important as physical infrastructure.
- Environmental Compliance and ZLD Norms
- Pharmaceutical manufacturing can generate chemical waste and effluents. Stricter environmental rules, including Zero Liquid Discharge (ZLD) norms, have increased compliance costs.
- While environmental protection is essential, many MSMEs may require financial and technical support to shift towards cleaner production.
- Talent Deficit in Advanced Technologies
- India faces a shortage of skilled professionals in areas such as bioprocessing, genomics, mRNA technology, clinical bioinformatics and AI-led drug design.
- Traditional pharmacy education does not fully meet the needs of modern biopharma. This skill gap can slow India’s movement into advanced therapies.
- Intellectual Property and Trade Frictions
- India’s strict patent standards, especially its resistance to evergreening, protect public health and affordable access. However, multinational companies often view these provisions as barriers to innovation investment.
- India must balance two objectives:
protecting affordable access to medicines and encouraging genuine innovation.
Measures Needed to Strengthen India’s Pharmaceutical Sector
- Build Predictive Regulatory Sandboxes
- India should create regulatory sandboxes for emerging therapies like CAR-T therapy, CRISPR-based treatments and mRNA platforms. These sandboxes can allow controlled testing under close regulatory supervision.
- This will help India regulate new technologies without delaying innovation.
- Adopt Continuous Quality Monitoring
- India should move from periodic inspections to Continuous Quality Monitoring. Modern factories can use IoT-enabled systems to track quality in real time.
- This will improve trust in Indian products and reduce the risk of global regulatory action.
- Strengthen Global Regulatory Harmonisation
- India should align its standards with global systems such as the Pharmaceutical Inspection Co-operation Scheme (PIC/S). Mutual recognition with trusted regulators can reduce repeated inspections and improve market access.
- Regulatory harmonisation will make India more competitive in premium markets.
- Create a Quad-Helix Innovation Ecosystem
India needs collaboration among four key actors:
- Government
- Industry
- Academia
- Venture capital
This Quad-Helix model can support high-risk research and help convert laboratory ideas into market-ready medicines.
A National Innovation Fund can provide patient capital for New Chemical Entities and advanced therapies.
- Promote Green Chemistry and Circular Economy
- India should promote flow chemistry, continuous manufacturing, solvent recovery and resource efficiency. These methods reduce waste and improve productivity.
- Specialised pharma parks with common effluent treatment plants can help MSMEs meet environmental standards at lower cost.
- Develop Pharma-Bio-Data Talent
- India should create specialised training programmes in molecular biology, chemical engineering, computational biology, clinical bioinformatics and regulatory science.
- Pharmacy education must be linked with industry needs. Students should get practical exposure through clinical-ready certifications and industry immersion.
- Use AI and Blockchain for Pharma Governance
- AI can support drug discovery, clinical trial design and manufacturing efficiency. Blockchain can help track medicines across the supply chain and reduce counterfeit drugs.
- Digital twins can be used to predict equipment failure and improve production planning.
- Strengthen India’s Global Pharma Brand
- India should build a strong global brand based on quality, affordability, reliability and ethical manufacturing.
- Mutual Recognition Agreements and global distribution hubs can improve India’s access to high-value markets.
- Shift towards Value-Based Pricing
- India should explore value-based pricing, where the price of a medicine reflects its clinical benefit and long-term social value.
- Price-volume agreements can help maintain affordability while giving manufacturers predictable revenue for innovation.
Way Forward
- India’s pharmaceutical sector needs a balanced strategy. It must protect its strength in affordable generics while also investing in advanced innovation. Domestic API production should be expanded, especially in fermentation-based KSMs and life-saving antibiotics.
- Regulatory reform should focus on speed, transparency and global trust. Faster approvals should not compromise public safety. Therefore, digital approvals, risk-based inspections and continuous quality monitoring must become standard practice.
- India should also support MSMEs in meeting environmental and quality standards. Common infrastructure in pharma parks, financial incentives for ZLD compliance and technology support can make the transition smoother.
- Finally, India must treat pharmaceutical innovation as a strategic national priority. With strong R&D, skilled talent, trusted regulation and sustainable production, India can become a resilient and science-led anchor of global healthcare security by 2030.
Conclusion
India’s pharmaceutical sector is moving from a low-cost generic model to a high-value innovation model. This transition will depend on strong regulation, better R&D, skilled talent, supply-chain autonomy and global quality trust.
Schemes such as Biopharma Shakti, PLI support for APIs, regulatory modernisation by CDSCO and the expansion of biosimilars show that India is preparing for the next stage of pharmaceutical growth.
However, challenges such as API dependence, quality concerns, weak R&D investment, environmental compliance costs and talent shortages must be addressed urgently. If India harmonises global standards with domestic innovation, it can strengthen its pharmaceutical sovereignty and emerge as a trusted global healthcare leader by 2030.
UPSC PYQ
Q. Consider the following statements about the Bureau of Pharma PSUs of India (BPPI):
(CDS-I, 2019)
- It is the implementing agency of Pradhan Mantri Bhartiya Janaushadhi Pariyojana (PMBJP).
- It has been registered as an independent society under the Societies Registration Act, 1860.
Which of the statements given above is/are correct?
A. 1 only
B. 2 only
C. Both 1 and 2
D. Neither 1 nor 2
Answer C. Both 1 and 2
Explanation
Statement 1 is correct
The Bureau of Pharma PSUs of India (BPPI) is the implementing agency of the Pradhan Mantri Bhartiya Janaushadhi Pariyojana (PMBJP).
It was established under the Department of Pharmaceuticals, Ministry of Chemicals and Fertilizers. Its main role is to coordinate the procurement, supply and marketing of quality generic medicines through Janaushadhi Kendras.
Statement 2 is correct
BPPI was registered as an independent society under the Societies Registration Act, 1860 in April 2010.
This gave it a separate legal identity for carrying out the work related to the Janaushadhi scheme.
CARE MCQ
Q. Consider the following in the context of India’s pharmaceutical sector:
- Biopharma Shakti
- Production Linked Incentive Scheme
- SUGAM Portal
- Jan Aushadhi Kendras
Which of the above are associated with strengthening India’s pharmaceutical and healthcare ecosystem?
A. 1, 2 and 3 only
B. 2 and 4 only
C. 1, 3 and 4 only
D. 1, 2, 3 and 4
Answer: D
Explanation:
- Biopharma Shakti: Supports biopharmaceutical innovation and research infrastructure.
- PLI Scheme: Encourages domestic production of APIs and pharmaceutical components.
- SUGAM Portal: Supports digital regulatory processes and faster approvals.
- Jan Aushadhi Kendras: Improve access to affordable medicines.
Additional Information:
India’s pharma strategy combines global competitiveness with domestic affordability.
FAQs
Q. What are Active Pharmaceutical Ingredients?
Active Pharmaceutical Ingredients are the main active substances in medicines that produce the intended therapeutic effect.
Q. Why is API dependence a concern for India?
API dependence is a concern because disruptions in imports can affect the production of essential medicines and weaken health security.
Q. What is Biopharma Shakti?
Biopharma Shakti is a major initiative aimed at strengthening India’s biopharmaceutical innovation ecosystem through research institutions and clinical trial infrastructure.
Q. Why are smarter regulations important for pharma growth?
Smarter regulations reduce delays, improve safety, build global trust and help Indian companies access high-value regulated markets.
Q. What is Zero Liquid Discharge?
Zero Liquid Discharge is an environmental system in which industrial wastewater is treated and reused so that no untreated liquid waste is discharged into the environment.
Relevance: UPSC: GS Paper II – Health, Governance, Public Health Systems, International Health Regulations
For Prelims:
Hantavirus, Zoonotic Spillover, One Health, Wildlife Reservoirs, Aedes aegypti, Aedes albopictus, Anopheline Mosquitoes, Nipah Virus, Ebola, Filoviruses, Coronaviruses, International Health Regulations, Pandemic Accord.
For Mains:
Zoonotic Risk, Climate Change and Health, Human-Wildlife Interface, Disease Surveillance, Biosecurity, Public Health Preparedness, One Health Governance, Habitat Fragmentation, Industrial Livestock Farming, Global Health Security.
Why in News?
- A recent hantavirus outbreak has renewed concern over zoonotic spillovers, where pathogens move from animals to humans.
- Experts have highlighted that such outbreaks may become more common due to deforestation, climate change, human expansion into wildlife habitats, industrial farming and global travel.
- The issue is important because the conditions that allow animal-borne infections to emerge and spread are increasing rapidly.
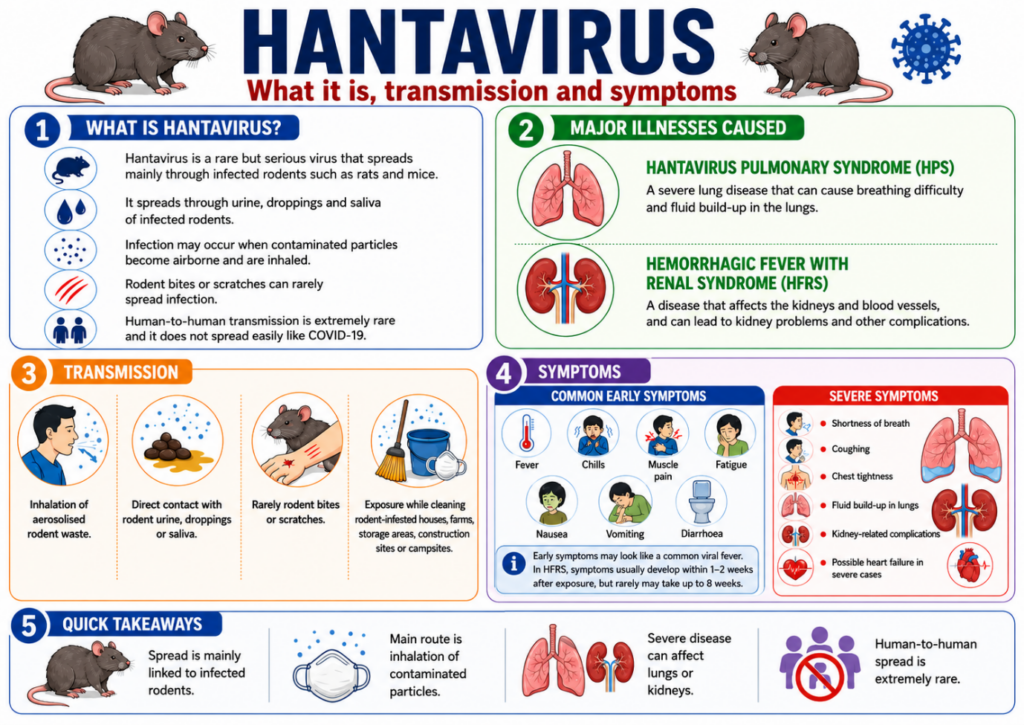
What are Zoonotic Spillovers?
- Zoonotic spillover refers to the transmission of pathogens from animals to humans.
- These pathogens may include viruses, bacteria or other disease-causing organisms.
- Spillovers are not completely random. They are often linked to ecological and social conditions that bring humans, domestic animals and wildlife into closer contact.
- COVID-19, Nipah, Ebola and hantavirus-like outbreaks show the public health risks of animal-origin infections.
What is a virus? A virus is a very small infectious particle that can cause disease in living organisms. Viruses are much smaller than bacteria. They cannot be seen with a normal microscope. They can infect humans, animals, plants and even bacteria. A virus is made up of:
Viruses cannot live and multiply on their own. They do not have their own machinery to make energy or proteins. So, they enter a living cell and use the cell’s machinery to make more viruses. That is why viruses are called intracellular parasites, meaning they live and multiply inside living cells. |
Why Spillovers May Become More Frequent
- Deforestation brings humans closer to wildlife reservoirs.
- Agricultural encroachment increases contact between farms and animal habitats.
- Unplanned urban growth expands cities into wildlife zones.
- Global travel and trade allow local outbreaks to spread rapidly.
- Climate change alters animal movement, vector distribution and disease geography.
- The list of pathogens with spillover potential is large, including filoviruses, influenza viruses and coronaviruses.
Major Human-Animal Interaction Risks
1. Industrial Livestock Farming
- Industrial farming creates large concentrations of genetically similar animals.
- Such conditions can amplify pathogens with pandemic potential.
- Influenza is one of the clearest examples.
- Weak bio-surveillance in animal production systems can increase risk.
2. Deforestation and Habitat Fragmentation
- Habitat loss pushes bats, rodents and other reservoir hosts into human-modified landscapes.
- Outbreaks such as Nipah in India, Malaysia and Bangladesh and Ebola in Central Africa show this pattern.
- Forest loss increases direct and indirect human-wildlife contact.
Surveillance Gaps
- Current disease surveillance systems are still more focused on responding to outbreaks than predicting them.
- Human clinical surveillance often detects disease only after people fall sick.
- Early warning systems need stronger:
- Veterinary surveillance
- Wildlife monitoring
- Environmental sampling
- Real-time data sharing
- A pathogen may circulate in animal reservoirs for years before a visible human outbreak occurs.
- One Health surveillance is therefore necessary because it connects human health, animal health and environmental health.
Role of Climate Change
- Climate change is reshaping the geography of zoonotic diseases.
- Mosquitoes such as Aedes aegypti and Aedes albopictus are expanding into new altitudes and latitudes.
- Tick distribution patterns are also changing.
- Anopheline mosquitoes are appearing at elevations where they were earlier absent.
- Changes in rainfall, temperature and land productivity affect animal behaviour and migration.
- Climate stress may alter bat roosting patterns and rodent populations.
- Fragile health systems face higher risk because they often lack capacity for early detection and response.
Why Zoonotic Diseases are a Major Public Health Challenge
- COVID-19 showed that zoonotic diseases can become global crises.
- Such diseases are shaped by the convergence of:
- Ecological disruption
- Climate change
- Globalisation
- Antimicrobial resistance in animal reservoirs
- Weak surveillance systems
- Preparedness gaps include limited manufacturing capacity, unequal access to countermeasures and weak global governance mechanisms.
- Zoonotic diseases are likely to remain a defining public health challenge of this century.
Examples of Zoonotic Diseases Zoonotic diseases are diseases that spread from animals to humans. Some important examples are:
Note – Zoonotic diseases can spread through animal bites, contaminated food or water, insects, close contact with animals, or exposure to animal waste. |
Significance
- Highlights the link between environment, animals and human health.
- Shows the need for the One Health approach in disease prevention.
- Connects climate change with public health risks.
- Emphasises the importance of early detection before human outbreaks occur.
- Underlines the role of wildlife and veterinary surveillance.
- Strengthens the case for better pandemic preparedness.
- Shows that environmental degradation can become a health security issue.
Challenges
- Surveillance systems are still largely human-clinical and reactive.
- Wildlife and veterinary monitoring remain underfunded and fragmented.
- Deforestation and habitat loss continue to increase human-wildlife contact.
- Industrial livestock systems may amplify pathogens.
- Climate change is expanding disease-vector ranges.
- Fragile health systems may not detect new outbreaks early.
- Global travel reduces the time available for containment.
- International reporting systems may suffer from weak compliance and delayed alerts.
Way Forward
- Strengthen integrated One Health surveillance across human, animal and environmental systems.
- Improve veterinary and wildlife disease monitoring.
- Create standardised protocols and real-time data sharing mechanisms.
- Regulate industrial livestock farming with stronger bio-surveillance.
- Reduce deforestation and habitat fragmentation.
- Strengthen climate-sensitive disease surveillance.
- Improve early reporting under International Health Regulations.
- Use the Pandemic Accord process to strengthen global preparedness and cooperation.
- Build public health capacity in vulnerable and climate-exposed regions.
UPSC PYQ
Q. Which one among the following pairs of diseases and their types is not correctly matched? (CDS-2026 )
A. Polio — Viral disease
B. Athlete’s foot — Fungal disease
C. Dengue fever — Non-viral disease
D. Whooping cough — Bacterial disease
Answer: C
Explanation
The pair in Option C is not correctly matched because Dengue fever is a viral disease, not a non-viral disease.
Dengue is caused by the Dengue virus (DENV). It spreads mainly through the bite of infected Aedes mosquitoes, especially Aedes aegypti.
- Polio — Viral disease: Correct
Polio is caused by the Poliovirus. It mainly affects the nervous system and can lead to paralysis in severe cases. - Athlete’s foot — Fungal disease: Correct
Athlete’s foot is a fungal infection of the skin, usually affecting the feet. It is also called Tinea pedis. - Dengue fever — Non-viral disease: Incorrect
Dengue fever is a viral disease caused by the Dengue virus. Hence, calling it a non-viral disease is wrong. - Whooping cough — Bacterial disease: Correct
Whooping cough, also called Pertussis, is caused by the bacterium Bordetella pertussis.
Additional Information
Diseases can be classified based on their causative agents:
Type of Disease | Examples |
Viral diseases | Polio, Dengue, COVID-19, Measles |
Bacterial diseases | Tuberculosis, Cholera, Whooping cough, Typhoid |
Fungal diseases | Athlete’s foot, Ringworm |
Protozoan diseases | Malaria, Amoebiasis |
CARE MCQ
Q. Consider the following diseases in the context of zoonotic diseases:
- Rabies
- Nipah
- Ebola
- Brucellosis
Which of the above are examples of zoonotic diseases?
A. 1 and 2 only
B. 1, 2 and 3 only
C. 2, 3 and 4 only
D. 1, 2, 3 and 4
Answer: D
Explanation:
- Rabies – Correct. Rabies is a zoonotic disease transmitted between animals and humans.
- Nipah – Correct. Nipah is also an example of a zoonotic disease.
- Ebola – Correct. Ebola is included among zoonotic diseases.
- Brucellosis – Correct. Brucellosis is another zoonotic disease mentioned in the content.
Additional Information:
Zoonotic diseases are infectious diseases transmitted between animals and humans. They can be caused by:
- bacteria
- viruses
- parasites
- fungi
The given content also notes that climate change and land-use changes increase human-animal interaction and raise the risk of zoonotic spillovers.
FAQs
Q. What is zoonotic spillover?
Zoonotic spillover is the transmission of pathogens from animals to humans.
Q. Why is hantavirus in news?
A recent hantavirus outbreak has raised concerns about rising zoonotic spillover risks.
Q. Why are zoonotic outbreaks increasing?
They may increase due to deforestation, human expansion into wildlife habitats, industrial farming, climate change and global travel.
Q. What is the One Health approach?
One Health is an integrated approach that connects human health, animal health and environmental health.
Q. How does climate change affect zoonotic diseases?
Climate change alters vector ranges, animal movement, rainfall patterns and disease geography.





